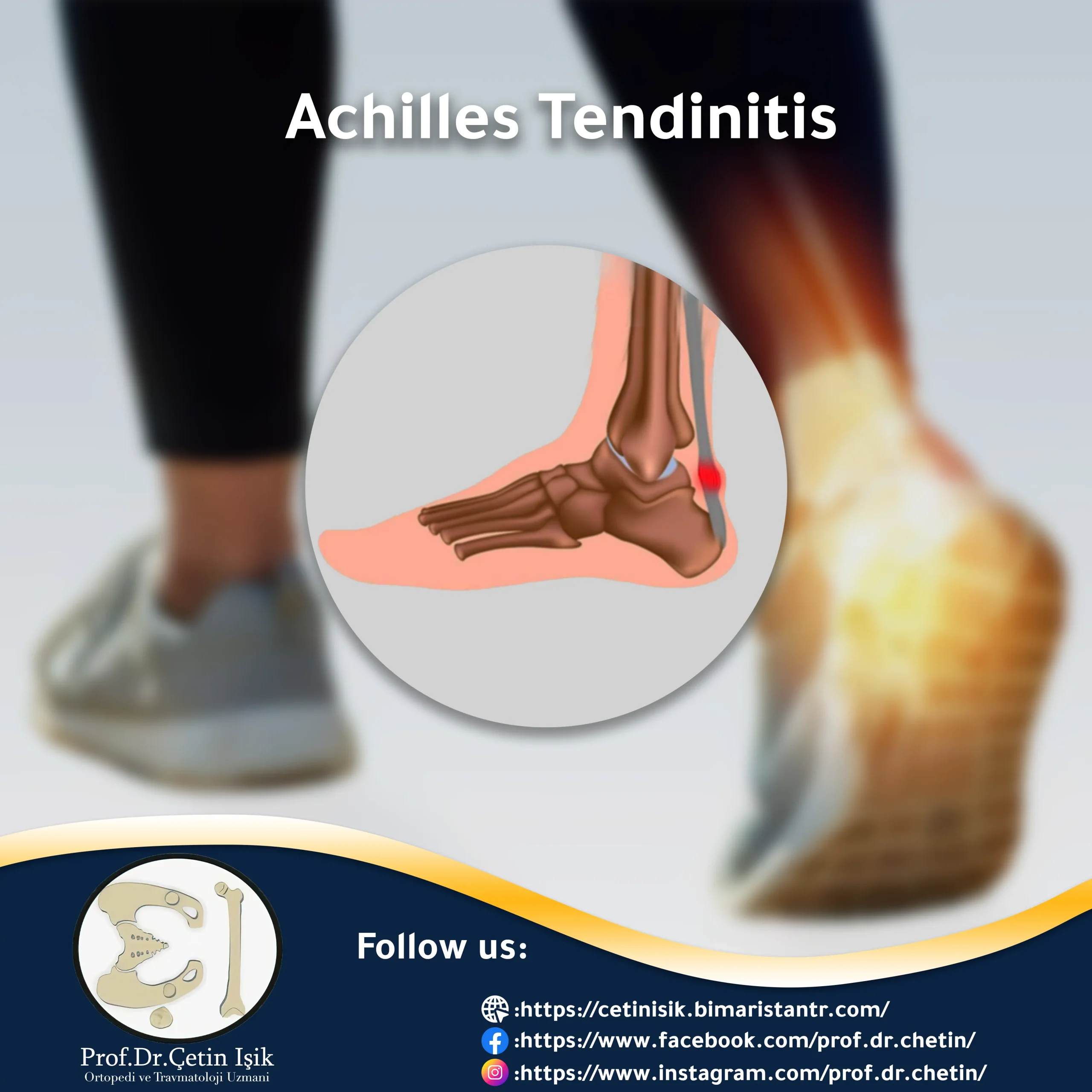
Achilles tendinitis is a common inflammatory injury in athletes. It causes pain, stiffness, and swelling of the Achilles tendon, which attaches the calf muscles to the heel bone at the back.
What is Achilles tendonitis?
Achilles tendinitis, or Achilles tendinopathy, occurs when the tendon becomes painful and swollen as a result of rupture or overuse, as in runners, and people who play sports such as tennis, which require a lot of sudden stops and turns.
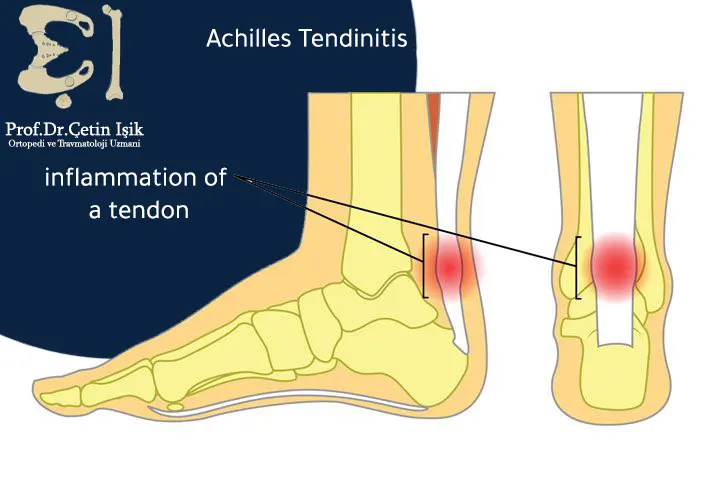
The Achilles tendon is the largest and strongest tendon in the human body, but it is the most vulnerable to damage due to its lack of flexibility and overuse. The leg is on the heel which is essential for walking or running.
The incidence of Achilles tendinitis is 24% in athletes, and the incidence is higher in the elderly, especially in men.
Types of Achilles tendinitis
The two types of Achilles tendonitis are classified according to the affected section of the tendon into:
- Insertional Achilles tendinitis: As the fibers in the middle of the tendon begin to thicken and swell, this type of inflammation affects younger, more active people.
- Insertional Achilles tendinitis: In the lower section of the tendon, where it attaches to the heel bone, where the blood supply is poor, it can occur in anyone regardless of their activity, yet it is common in overused people such as long-distance runners.
Causes of Achilles tendonitis
Achilles tendinitis is often caused by excessive exertion during exercise or gradual wear and tear with age, and tendon pain can also be caused by arthritis, especially in middle-aged and older adults.
Other predisposing causes of Achilles tendinitis include:
- Not warming up enough before exercising
- Repetitive movements that strain the calf
- Sudden increase in the intensity of physical activity without allowing the body to adapt
- Old or unsuitable shoes
- Wearing high heels daily for a long period of time
- The presence of a bony bump on the heel of the foot in the back, which causes friction with the tendon
- Flat feet
- The difference in the length of the legs
- Obesity, as excess weight places an additional burden on the foot
- Sprained ankle
Symptoms of Achilles tendonitis
The three main symptoms most commonly associated with Achilles tendinitis include:
Calf and heel pain:
It tends to be above the area of the tendinitis and sometimes extends to the calf. Achilles tendinitis pain usually gets worse in the morning upon waking or after a long rest, and the few steps at the beginning of walking are difficult and then the pain subsides after a few minutes as the Achilles tendon relaxes.
The pain associated with Achilles tendinitis usually begins as a mild pain, as it appears in the early stages of inflammation in strenuous work, while in the chronic stage it is in almost all activities and even in the period of rest at times.
Tendon thickness:
The patient often feels a lump at the site of the injury in the Achilles tendon, which can be painful to the touch, this varies depending on the severity and location of the inflammation.
Sclerosis:
In Achilles tendinitis, the ankle and leg become tight and stiff,which limiting movement of the foot. It also tends to be worse after long rest and relieved by slight movement.
If you have any of the symptoms of Achilles tendinitis, you can: Contact us To answer your questions.
Diagnosis of Achilles tendonitis
Both a medical history and a physical exam are required to diagnose Achilles tendinitis. The doctor also asks about the patient's symptoms and asks for an X-ray or ultrasound.
Physical examination:
A thorough physical examination of the foot and ankle can help determine the cause of Achilles tendinitis.
Important elements of the test include examining and applying pressure to the area around the tendon and checking for swelling, warmth, and thickness of the tendon. There may be a crackling sound as the tendon moves, or small bumps along its length that indicate fibrosis and scar tissue formation, and finally, bruising can be seen on the tendon if it ruptures.
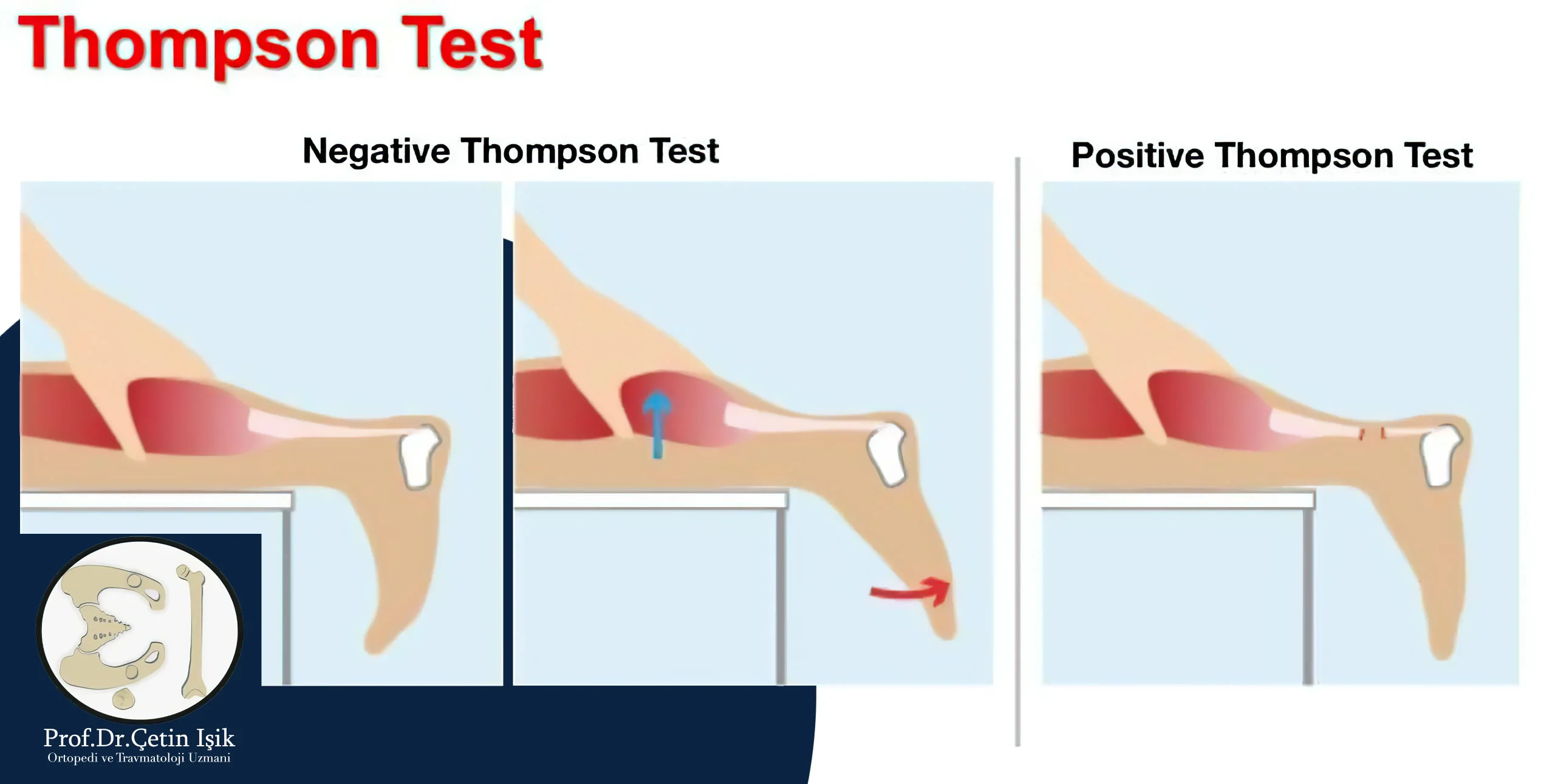
Thompson's test:
As part of diagnosing Achilles tendinitis, Doctor performs a Thompson's test which also called a calf compression test.
During this test, the affected person lies flat on the test table with their feet hanging over the edge of the table. The doctor applies pressure to the calf muscles in the back. The toes should be bent downwards. If this does not happen, the test is positive for Achilles tendinitis.
Radiography:
- X-ray of the heel bone: It detects calcifications in the proximal tendon and if there is a bony prominence above the heel, and can help rule out bone tumors.
- Ultrasound: Ultrasound detects thickening of the Achilles tendon and is also useful in the interventional treatment of tendinitis.
- Magnetic resonance imaging (MRI): It provides important information about the bone structure, and studies indicate that MRI is less sensitive than ultrasound to detect early changes in Achilles tendonitis.
Blood tests:
Blood tests may help if the doctor suspects that there is an infection in the heel bone or the skin of the back leg surrounding the Achilles tendon. An elevated white blood cell count can indicate inflammation, but it is not specific for Achilles tendinitis.
Achilles tendonitis treatment
There are several ways to treat Achilles tendinitis depending on the severity and age of the injury, requiring changes in the patient's activity level, sessions of physical therapy, taking medications and finally surgery.
Following and sticking to a treatment plan appropriate to the patient's condition is key to recovery , which includes the following:
Take adequate rest
It is not necessary to stop all activities in the case of Achilles tendonitis, however a change in activity is needed in response to muscle pain.
Ice compresses
Applying ice when pain starts or after exercise over the injury at the back of the heel may help reduce tendon swelling.
compression belts
Compression braces and straps are used to prevent the tendon from moving too much by wrapping it around the heel affected by Achilles tendinitis.
Orthopedic appliances
It can be used to correct foot deformities, such as flat feet, as it reduces the load on the heel and relieves pain that caused by inflammation.
Medications
To reduce pain and swelling caused by Achilles tendinitis, NSAIDs such as naproxen and ibuprofen can be taken.
Doctors do not recommend steroid injection to relieve pain in the case of Achilles tendonitis because of its long-term effects.
Achilles tendonitis physical therapy
Physiotherapy is one of the most important treatments for a full recovery, which may take three to six months.
It is a good idea to start with exercises that strengthen the calf muscles and the muscles around the tendon, under the supervision of a qualified trainer.
A deep massage of the calf muscles that attach to the Achilles tendon is an important helpful treatment option, and exercises that include toe raises and heel stabilization are also helpful.
Shock wave therapy
If the above measures are insufficient, extracorporeal shock wave therapy can reduce the pain rate up to 60% to 80% over a period of four weeks, using low-intensity sound waves that destroy tissue scars in the calf tendons.
Surgical treatment of Achilles tendonitis
The patient may resort to surgical treatment after conservative measures have failed for six months or if chronic Achilles tendinitis develops.
In some cases, an orthopedic surgeon can suggest surgical options based on various factors such as the severity of the injury, the patient's age and activity level, which include:
Tendon debridement and repair: If most of the Achilles tendon is healthy, the surgeon removes only the damaged portion and sews the two ends of the remaining healthy tendon together. After the procedure, the patient wears a supportive shoe for a few weeks.
Debridement with tendon transfer: If more than half of the Achilles tendon is damaged, the surgeon takes a graft from another tendon and moves it to the heel bone. The athlete may not be able to play their sport competitively after this procedure.
Hydrocision TenJet: In this minimally invasive ultrasound-guided technique, a high-speed saline solution is used to break up scar tissue in the Achilles tendon. The pressurized saline acts as a knife to selectively remove unhealthy tissue. This procedure is performed on an outpatient clinic rather than in a hospital.
To determine the best treatment for your injury; You can contact Dr Çetin Işık To answer your inquiry.
Prevention of Achilles tendonitis
To reduce the risk of developing Achilles tendinitis or Achilles tendinitis, follow these tips during daily life:
- A good warm-up before you start exercising, and start stretching and stretching exercises to tighten the calf muscles.
- Vary your exercise pattern to avoid repetitive stress on the Achilles tendon.
- Wear well-fitting supportive shoes
- Avoid running on flat ground as much as possible.
- If you notice symptoms of Achilles tendinitis such as pain, you should take a break and monitor the condition well.
Sources:
Common questions
Recovery from Achilles tendinitis tends to be slow, so recovery can take anywhere from three to six months, with adherence to treatment for Achilles tendinitis.
Achilles tendinitis is one of the most painful things, however, self-care and conservative measures such as rest, ice packs on the back of the heel, compression brace and pain medication are effective in treatment if adhered to, and surgery may be resorted to if it persists Pain and progression of Achilles tendinitis to a chronic condition or complications such as an Achilles tendon rupture.
It is generally a good idea to change activities from high intensity, such as running, to low intensity, such as walking short distances, as this will help speed the healing of Achilles tendinitis and reduce pain in the back of the leg and in the calf muscles.