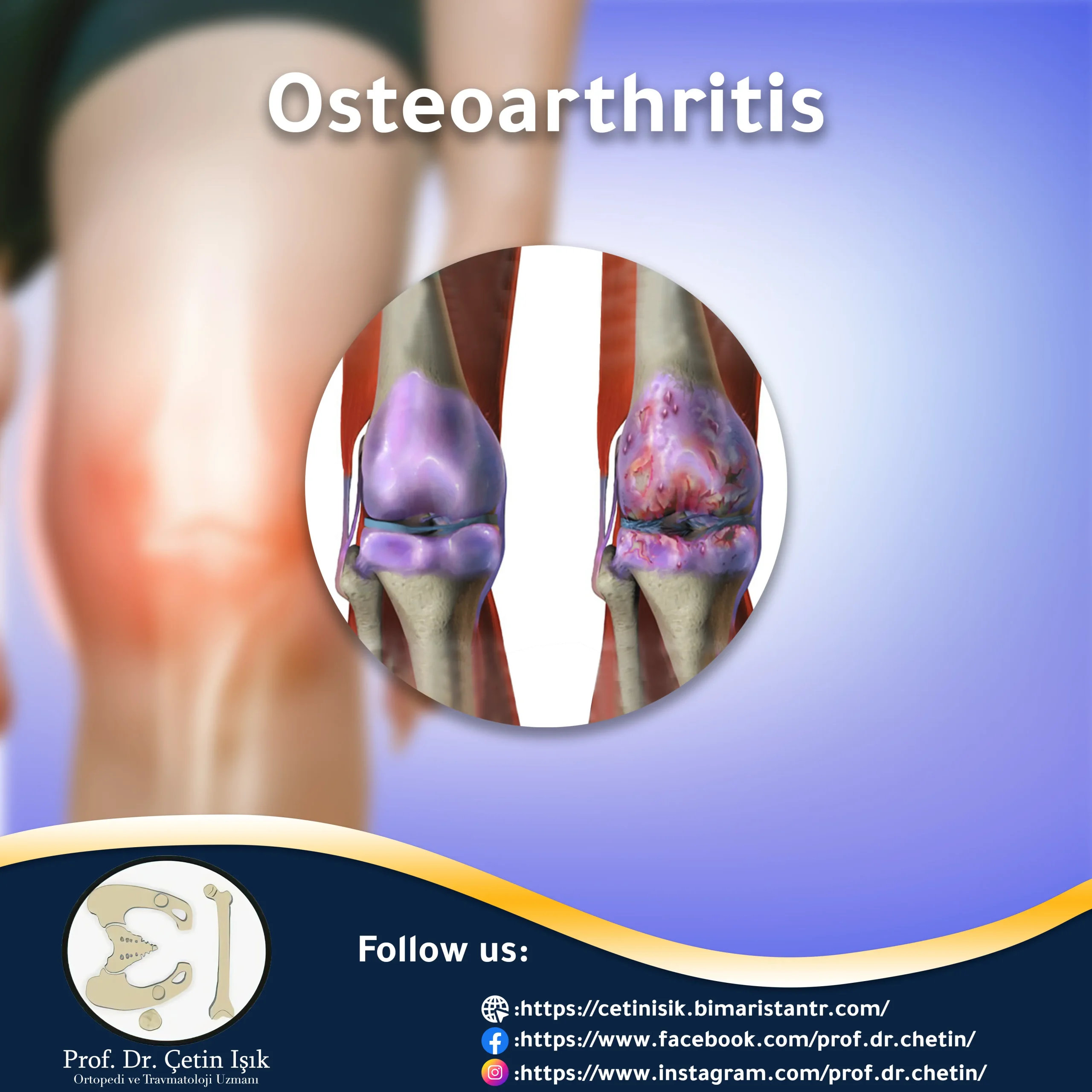
Osteoarthritis, also called degenerative arthritis, is one of the most common orthopedic diseases and is associated with mild symptoms at first, but neglecting the condition and delaying treatment may lead to bad consequences such as fractures and osteoporosis.
What is osteoarthritis?
Osteoarthritis is a degenerative disease that affects the joints and bones, meaning that the cartilage, bone tissue and surrounding ligaments are destroyed and damaged over time, and this is the most common cause of arthritis in the body, affecting millions around the world.
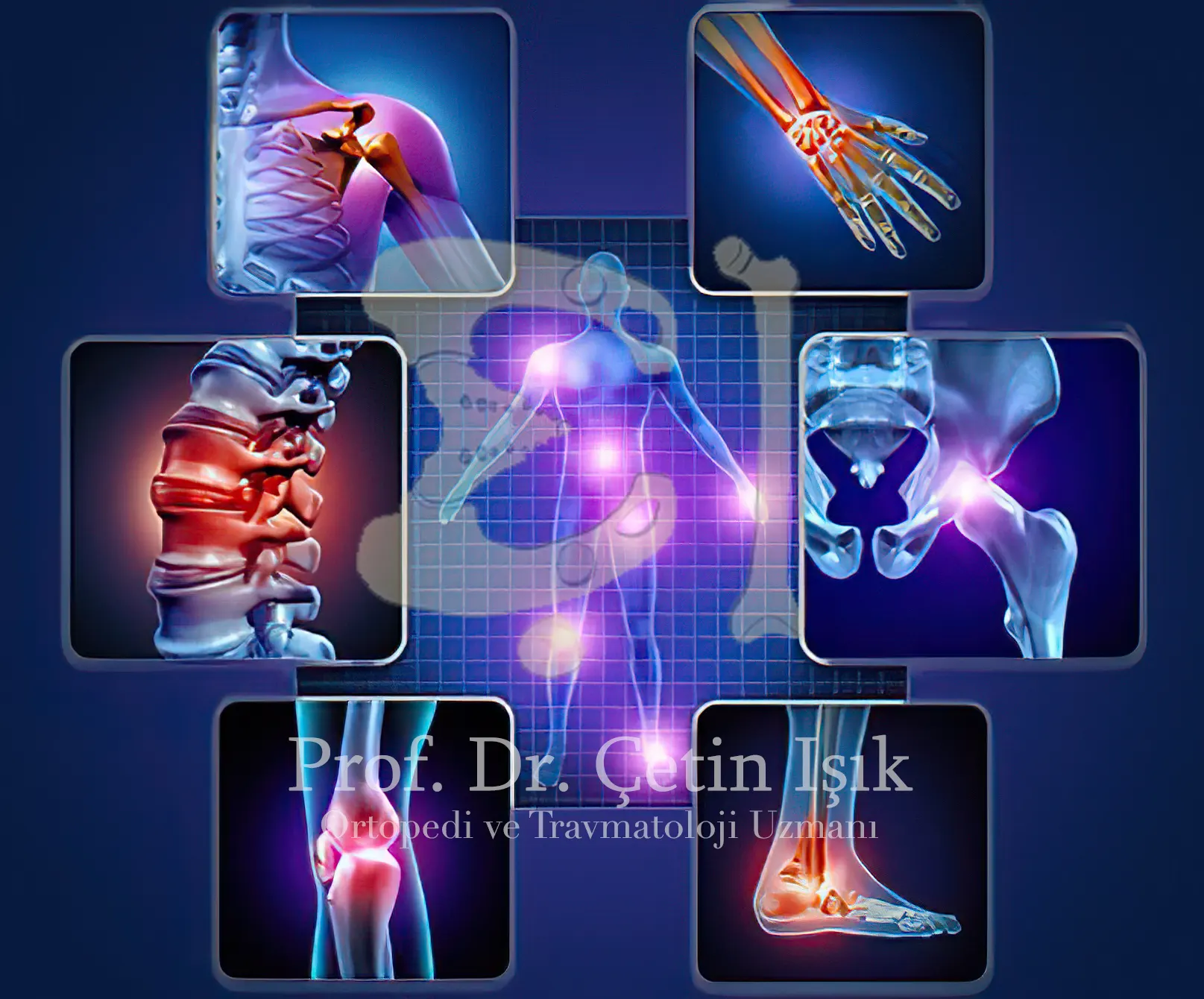
People with osteoarthritis complain of pain and stiffness in the affected joint when it has not been moved for a long time. It may affect specific joints most commonly:
- Knees
- Lumbar spine
- Hips
- The neck
- The joints in the hands and fingers
Read more about: Finger joint stiffness treatment.
The disease affects each patient according to a distinct articular pattern. It may be mild symptoms that do not affect daily activities and the pain can be controlled easily, or it may be severe as severe joint damage develops after several years.
Researchers have not been able to pinpoint the exact cause of osteoarthritis, which induces erosion of joint tissue, but it is well established that once it does appear, it will damage:
- Cartilage
- Ligaments
- Bones
- synovial membranes
- Tendons
When you feel pain and swelling in your knee, for example, you will definitely become less active, this usually causes weakness of the muscles surrounding the joint, which is associated with increased pressure on the injured joint that was supported by these muscles. .
Symptoms of osteoarthritis
It is possible for degenerative arthritis to affect anyone, but most of those affected are the elderly, and the disease is more prevalent among women, especially after the age of fifty, i.e. after menopause.
It is not excluded that young people will also develop osteoarthritis as a result of another genetic disease, joint injury or congenital deformity that causes long term damage.
Symptoms of osteoarthritis begin slowly, in one or a few joints at first. These symptoms include:
- Arthralgia that improves with rest, and chronic inflammation causes night pain that may be limited to the affected area or extend to large areas.
- Stiffness that lasts less than 30 minutes in the morning or after rest.
- Changes that limit movement in the joint.
- Swelling in and around the joint, especially where joint stress following sports is a major cause.
- Loss of joint stability.
Osteoarthritis of the thigh
Some may think that the thigh is one of the places where osteoarthritis occurs, but in fact, the thigh is a common place for osteoarthritis pain in the hip and knees, and this pain is not due to the disease occurring in the thigh bone itself, usually except in rare and advanced cases.
Osteoarthritis of the hand
It is noticed early as a result of deformation of the fingers of the hand after suffering from degenerative arthritis, and fortunately, this type of arthrosis can be easily treated because the affected joints are small in size.
Osteoarthritis of the hip
The hip bones are most commonly affected by osteoarthritis, where pain reaches the thigh, back, and sometimes the knees. Over time, these joints become severely limited in movement.
Osteoarthritis of the knee
A painful condition in which the patient hears a popping sound in the knees while walking. With time, the ligaments weaken, which leads to bending and deformation of the knee.
Osteoarthritis of the foot
Symptoms of osteoarthritis in the feet are more severe when wearing high heels or practicing strenuous sports such as running, where the feet make popping sounds that cause the patient to worry when walking.
Osteoarthritis of the spine
The patient may feel stiffness and pain in the lower back or neck. If the condition is neglected and not treated, a defect occurs in the structure of the vertebral canal called spinal stenosis, which may lead to neurological symptoms such as numbness and tingling.
Causes of osteoarthritis
Osteoarthritis occurs as a result of gradual damage to the joints. It is considered one of the most important diseases of the bones and joints, whose incidence increases with age, meaning the older the patient, the longer the joint is exposed to work pressure.
Other causes of joint damage include:
- Accidents such as cartilage tears, joint dislocations and ligament ruptures.
- Congenital joint deformity.
- Bad postures.
Also, risk factors that increase the risk of developing osteoarthritis include:
- A family member suffers from osteoarthritis
- Being a female patient
- Age over 50
- Menopause
- Occupations that require bending, climbing, or lifting heavy weights
- Accidents and injuries
- Obesity and being overweight
- Other diseases such as diabetes and rheumatoid arthritis
Diagnosis of osteoarthritis
There is no specific laboratory test to diagnose osteoarthritis and it is sometimes possible to:
- Giving a detailed medical history that includes the symptoms and other problems that the patient has suffered previously, in addition to the medications he is taking.
- Perform a thorough orthopedic examination.
- Imaging of the affected joints.
- Blood tests to roll out other causes of symptoms.
- Taking samples of joint fluid to look for other causes of joint pain, such as gout.
There are many modern bone imaging techniques that help doctors make a diagnosis, such as:
- X-rays: It shows the articular space and the location of the injured tissue in addition to the bony beaks, and the newly formed bone tissue does not appear on the simple image.
- MRI: It is the most accurate as it shows soft tissue damage in great detail and is more commonly used to confirm the diagnosis.

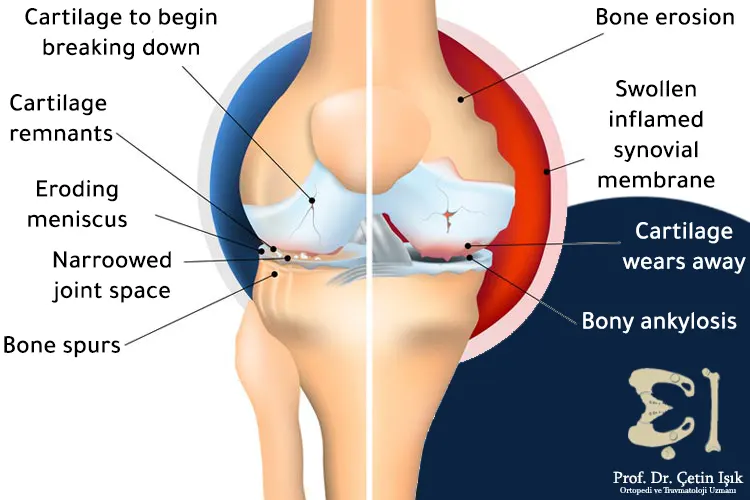
Image showing the space between normal bone and osteoarthritis on a radiograph
Osteoarthritis treatment
Osteoarthritis treatment aims to:
- Pain relief and relieving other symptoms
- Improve joint function
- Stop or slow down the course of the disease
- Maintaining an acceptable, healthy quality of life without hindrance
Therefore, this disease is not completely curable, and treatment methods focus on controlling symptoms and preventing progression of the disease.
Osteoarthritis medication treatment
Available in many forms, such as pills, syrups, patches, creams, and injections, they include:
- Pain killers: such as paracetamol and opioids that usually require a prescription.
- NSAIDs: These are the most commonly used and include aspirin, ibuprofen and naproxen, which can be taken without a prescription and are available in higher doses that require a prescription.
- Anti-irritants: Such as capsaicin and lidocaine ointments that relieve pain and give a refreshing feeling.
- steroids: This class of drugs works in a similar way to the anti-inflammatory hormone cortisol and is given orally or as an injection into the joint in the clinic.
- Platelet Rich Plasma: Plasma extract is injected into the joints to relieve the pain of osteoarthritis, but the US Food and Drug Administration has not declared its effectiveness and the evidence for its effectiveness is still weak.
- Other drugs: In cases of chronic pain, antidepressants such as duloxetine and anticonvulsants such as pregabalin are given.
Herbal treatment for osteoarthritis
Alternative therapies provide good options for patients whose symptoms are still mild and who can benefit from herbal materials and natural remedies by virtue of where they live as the people of India and South America.
In general, eating nuts that contain omega-3 fatty acids helps in relieving bone pain and degenerative arthritis, and nutritional supplements containing higher levels of omega-3s are more effective.
Green tea and ginger are among the most effective antioxidant and anti-inflammatory herbs that help manage osteoarthritis.
Surgical treatment of osteoarthritis
Some severe cases of osteoarthritis require surgery and patients usually resort to it only after all drug treatments have failed or a joint has been severely damaged.
Surgery does not guarantee improvement in osteoarthritis symptoms, but it may sometimes be the only option, and many patients have found improvement after it.
Joints that suffer from osteoarthritis can be largely replaced with titanium or aluminum prosthetic joints and the prosthetic joint may remain for 20 years without problems but eventually it must be replaced.
If the patient does not want to replace his joints, he can undergo joint fusion surgery instead, where the surgeon attaches the two ends of the joint to each other, which leads to permanently relieving the symptoms of degenerative arthritis.
Osteoarthritis and its complications
It is known that arthritis, especially osteoarthritis, is one of the most common bone diseases that cause problems and complications, especially degenerative ones. There may be psychological trauma after the injury, as it continues even after the joint disease itself has healed.
Physical complications include:
- Sleep problems
- Weight gain
- Osteonecrosis
- The disintegration of ligaments and tendons
- Hairy bone fractures
- Joint bleeding
Don't hesitate to Contact us Learn more about osteoarthritis and its treatments.
Sources:
- Arthritis Foundation
- National Institute of Arthritis and Musculoskeletal and Skin Diseases
- Medline Plus
- American Collage of Rheumatology
- National Health System UK
Common questions
The most effective way is to exercise, maintain fitness and lose weight.
Osteoarthritis does not have a direct cause, but there are risk factors and triggers.
Osteoarthritis is a condition of arthritis that results from the wear and tear of joint cartilage with age. Arthritis in general has many causes.
Degenerative osteoarthritis is a progressive disease with time. If it is not treated, symptoms will worsen, pain will become more severe, and the patient may eventually need a joint replacement.