Arthritis injections are many and varied. The most famous is steroid injections. All these injections are given inside the joint, except for antibiotics.
Arthritis injections are very useful in relieving pain and reducing joint swelling. The patient cannot take these injections himself. The doctor injects them into the affected joint using local anesthetics before starting the procedure. Learn about the most important types of these injections.
Corticosteroid injections are the best for arthritis
In some cases, the doctor may use arthritis injections that contain a combination of steroids and local anesthetics. Corticosteroid injections are helpful for patients with severe pain or inflammation who need prompt treatment. It is good to know that steroids can be injected into almost all joints of the body, such as:
- Ankle
- Elbow
- Knee
- Hip
- Shoulders
- The small joints of the hand, feet, spine, and wrist
This injection provides safe and effective pain relief and reduces inflammation. Pain and flare may occur at the injection site but it disappears within two days. The analgesic effect usually lasts 1 month, but there are long-acting medications that last 3 months.
Repeated intra-articular steroid injections lead to deterioration and damage to the joint cartilage and weaken the ligaments and tendons around the joint.
Intra-articular hyaluronic acid injection
Hyaluronic acid is one of the arthritis injections. It is a lubricating substance found naturally in the joint, but it decreases in: Degenerative arthritis. Hyaluronic acid can be injected into the patient's joints to compensate for its deficiency. The patient is usually given an injection every week for 3 or 5 weeks.
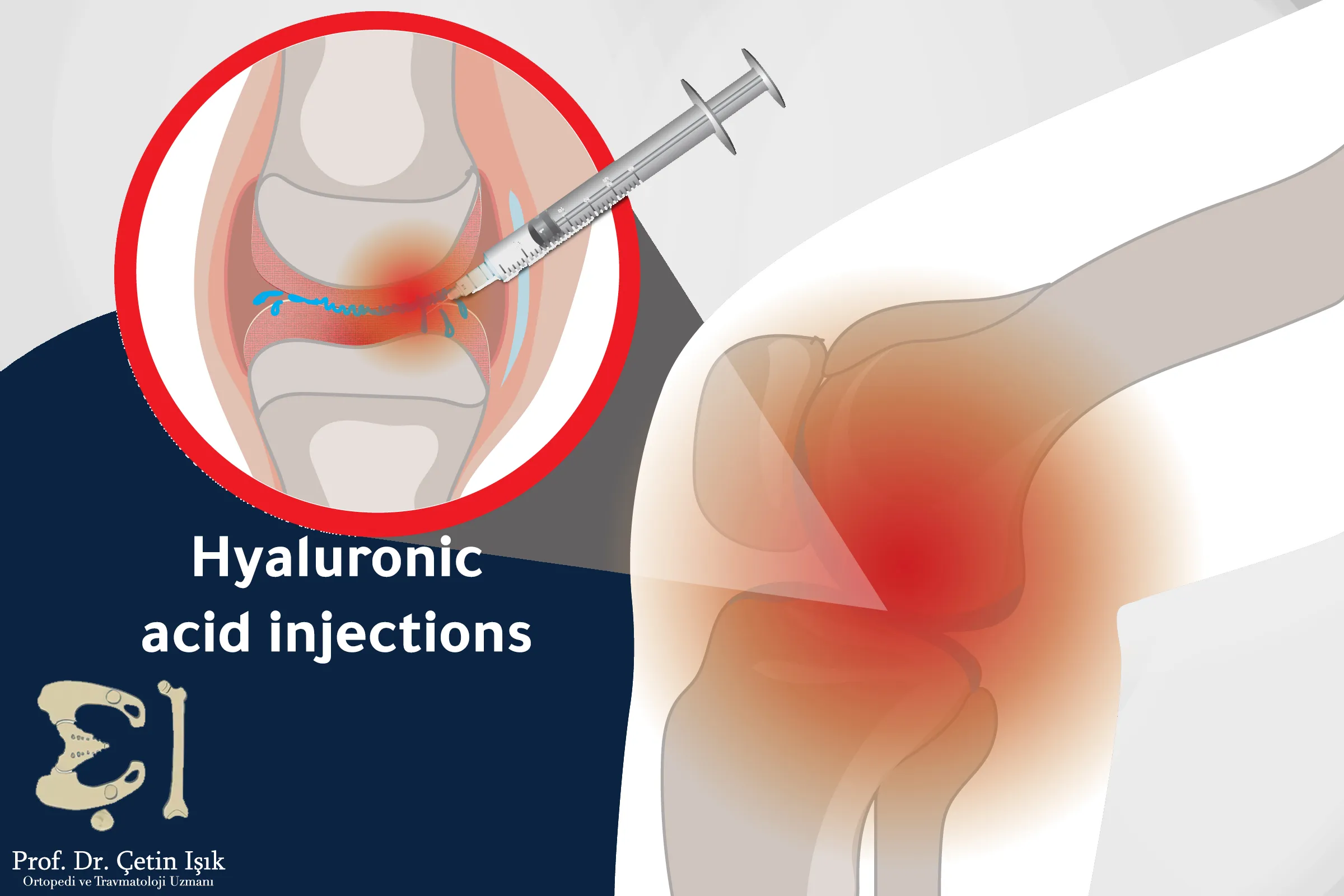
Although some studies do not support the administration of these injections, many doctors still recommend their use and find that repeated administration of hyaluronic acid helps reduce pain and joint stiffness.
Hyaluronic acid injections are safer and more tolerated than steroid injections because they have fewer side effects and give pain relief for 6 months.
The most common side effects include pain, swelling, and stiffness in the joint and the area around it. These injections have been approved by the US Food and Drug Administration (FDA) for use in the knee joint, but they are also used in the shoulder and hip.
stimulate healing via Prolotherapy injections
Prolotherapy involves injections containing irritating substances (usually a sugar solution) into the affected joint, ligaments, and tendons. The doctor injects 15 to 20 injections per month for 3 to 4 months.
The treatment principle is based on the theory that these irritating substances stimulate local healing of tissue damage in the area of injection.
This method is helpful for patients with degenerative arthritis who have not responded to physical therapy and weight loss. This method can also be used in all joints, but it is most successful in the joints of the lower back, fingers, and knees.
Platelet-rich plasma
Platelet-rich plasma (PRP) is one of the newer types of arthritis injections. Its effect is most significant in patients with mild to moderate degenerative arthritis.
Plasma is obtained by taking an appropriate amount of the patient's blood and processing it to extract the platelet-rich plasma, then injecting it into the painful joint of the patient himself. This injected substance is rich in platelets, anti-inflammatory, and immune-modulating proteins and is used once without repeating or given as an injection weekly for 3 weeks.
Several studies have revealed the benefit of this method in relieving pain and reducing stiffness, but its long-term effectiveness is unknown. In addition to that, it does not help with cartilage and tissue regeneration. Still, its pain-relieving effect is longer than that of steroids and is similar to or even better than that of hyaluronic acid injections.
Side effects of PRP injections are very rare, but the patient may feel some pain at the injection site.
Autologous conditioned serum
Autologous conditioned serum is used in arthritis injections. It is prepared by taking a blood sample from the patient and placing it in a special container (usually overnight), increasing anti-inflammatory molecules.
The next day, the doctor injects ACS into the joint to relieve pain and improve function. This injection is very beneficial for patients with moderate arthritis.
Doctors follow several protocols. This injection may be given once without repeating, once every week for 3 to 5 weeks, or twice a week for three weeks.
This injection is safe, effective, and non-irritating to the patient, but it does not help regenerate cartilage. It is used for muscles, tendons, and ligaments more than arthritis. Moreover, its side effects are rare, but swelling and bruising may occur at the injection site.
Stem cell injection or autologous fat injection
Stem cells can be obtained from the patient, either from bone marrow or adipose tissue, for arthritis injections. After taking the sample from the patient, we centrifuge it and extract the stem cells. Then we inject them into the patient's painful joint.
This treatment is based on the saying that stem cell injections will start the process of self-renewal of cartilage and tissue directly, but this has never been proven. Despite this, some studies have shown that this injection relieves the patient from pain and improves symptoms. It is believed that this is due to the effect of anti-inflammatory chemicals released by the bone marrow or fatty tissue in the sample.
These anti-inflammatory molecules are the same as those in platelet-rich plasma and autologous serum. Since sampling from fatty tissue or bone marrow is an invasive procedure, the previous methods are preferred over autologous stem cell injection unless the patient undergoes surgery.
Stem cells can be injected into all joints, but they are most commonly used in the knee.
Relieving joint pressure through puncture
Joint fluid puncture is a different type of injection for arthritis because it does not require any substance to be injected into the joint and is an easy and inexpensive procedure for the patient. Puncture involves inserting a needle into the joint cavity to remove excess fluid that causes pressure within the joint. This reduces swelling and stress, thus reducing pain, reducing stiffness and increasing flexibility.
The doctor may use the echocardiogram to guide the needle into the joint cavity if the joint is deeply positioned. Furthermore, the doctor may send a sample of the fluid extracted to be examined in a laboratory to find out the cause, such as infectionGout, and other types of arthritis. This procedure is considered a therapeutic and diagnostic method simultaneously.
The puncture can be repeated if the fluid collects again.
Puncture damage is rare, the most important of which is joint infection. Also, slight bleeding may occur after the procedure if the patient suffers from coagulation diseases such as hemophilia. Anesthetics should not be used if the patient is sensitive to them. The doctor can puncture all joints except for the pivotal joints (joints in the spine and rib cage).
We discussed the most important materials used in Arthritis injections and their benefits. The doctor can determine the appropriate injections according to the patient's condition and inject them himself in the clinic, which helps the patient a lot and relieves him of pain.
Sources:
Common questions
Intra-articular steroid injections are best, so they are used to relieve severe pain.
Arthritis injections may cause mild pain, so topical anesthetics are used before the injection.
Yes, but it is used intravenously in the case of septic arthritis caused by bacteria. Among the most important antibiotics used are vancomycin, ceftriaxone, and ceftazidime.
Penicillin injections were previously used, but now they have been discontinued due to the emergence of other more effective drugs.